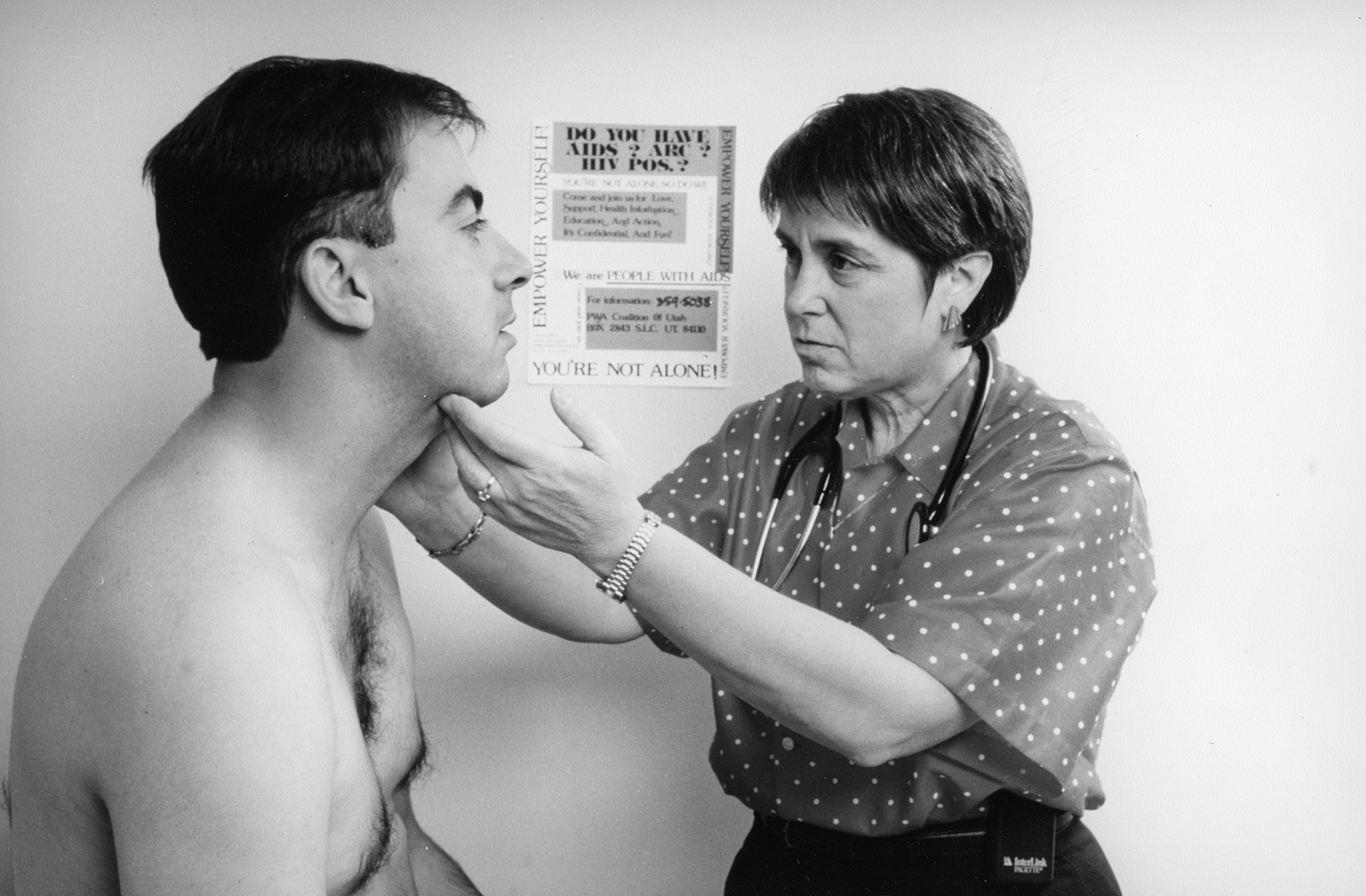
A Practice of Human Kindness
When the AIDS crisis erupted in Utah in the early 1980s, Kristen Ries was the only doctor in the state willing to care for HIV-positive patients. Four decades later, her efforts resonate in the lives she saved, and in the stories of people she cared for when no one else would.